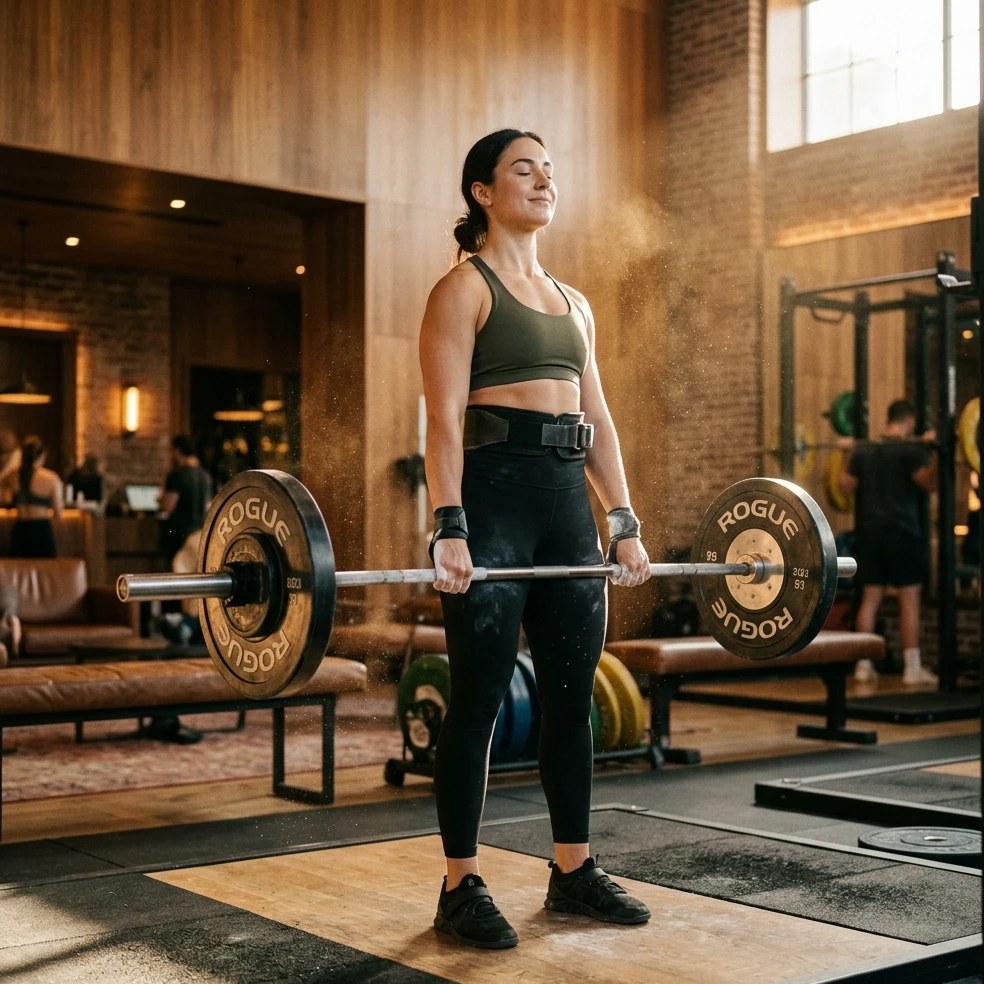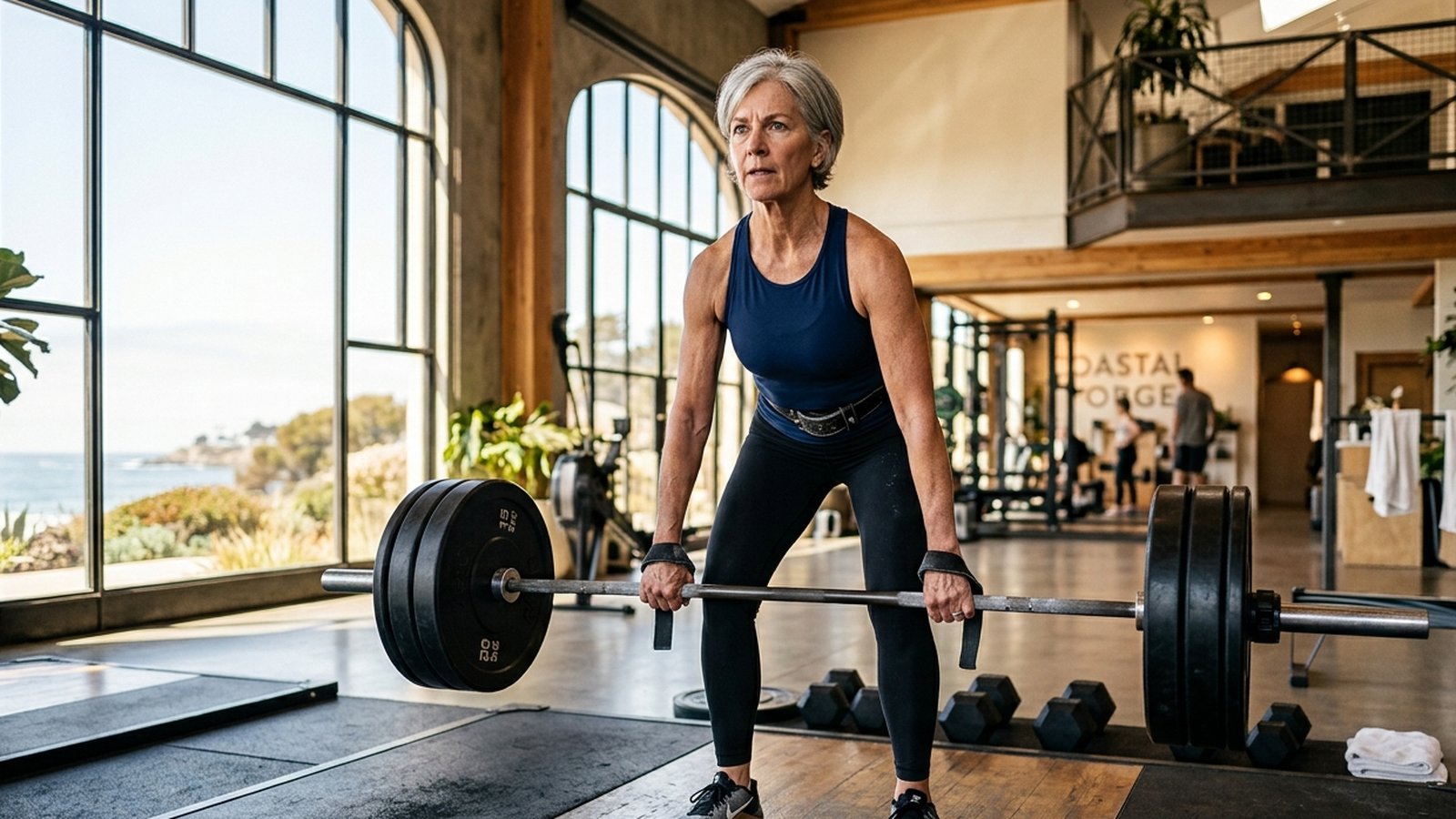The 60-second version
Resistance training has accumulated, in the last decade, the strongest mental-health evidence of any single movement modality. The 2018 Gordon meta-analysis of 33 RCTs (1,877 adults) showed resistance training reduced anxiety symptoms by an effect size of 0.31 — comparable to first-line pharmacological treatments for generalized anxiety disorder, with no side-effect profile. The 2018 Schuch meta-analysis on depression went further: 25 RCTs, 1,487 adults, effect size 0.66 in clinical depression. Mechanism evidence is converging on three pathways: HPA-axis recalibration (cortisol rhythm normalization), BDNF-driven neuroplasticity, and self-efficacy via measurable progress. The dose-response is clearer than for many drug interventions: 2–3 weekly sessions of moderate-intensity resistance training, sustained over 8–12 weeks, produces detectable benefit in most adults. The article walks through what the evidence supports, who benefits most, the realistic timelines, and the cases where lifting is not enough on its own.
Why lifting specifically — vs cardio
The popular framing has been “exercise helps mental health,” without specifying type. The 2010s and 2020s evidence shifted that. Resistance training has accumulated mental-health-specific evidence that — per dose — matches or exceeds aerobic exercise for anxiety and depression outcomes. The 2018 Gordon et al. meta-analysis pooled 33 RCTs of resistance training as the primary intervention for anxiety symptoms (not as adjunct to pharmacology). Findings:
- Effect size 0.31 (Cohen’s d) on anxiety symptoms across the pooled trials.
- Both clinical and subclinical anxiety populations responded.
- No dose-response above ~3 weekly sessions — more isn’t better past that point.
- Effect was independent of cardiovascular fitness changes Gordon 2017.
The 2018 Schuch et al. meta-analysis on depression similarly showed resistance training producing effect sizes of 0.66 (large) in clinical depression populations — comparable to many SSRIs and ahead of most psychotherapy modalities Schuch 2017. The 2023 Singh meta-analysis of 97 reviews of physical activity for mental health found resistance training and high-intensity interval training as the two highest-effect-size modalities for depression and anxiety Singh 2023.
“Resistance training, as primary intervention, produces clinically meaningful reductions in anxiety symptoms across both clinical and non-clinical populations. Effect sizes are comparable to first-line pharmacological treatments. No identified subgroup fails to benefit, though the magnitude varies.”
— Gordon et al., Sports Med., 2017 view source
The three converging mechanisms
| Mechanism | What it does |
|---|---|
| HPA-axis recalibration | Heavy training acutely spikes cortisol then crashes it; chronic adaptation reduces baseline reactivity to non-training stressors. Anxiety populations show flatter, more dysregulated cortisol rhythms; resistance training partially normalizes these. |
| BDNF and neuroplasticity | Brain-derived neurotrophic factor rises acutely with exercise. BDNF supports hippocampal neurogenesis and synaptic plasticity. Hippocampal volume is reduced in major depression; BDNF-driven recovery correlates with symptom reduction. |
| Self-efficacy through measurable progress | Strength gains in 4–8 weeks are observable, quantifiable, and outside normal life’s ambiguity. The objective “I lifted more than last week” signal builds general self-efficacy that transfers to other domains. Particularly potent in adults with depression who often experience global helplessness. |
| Sleep improvement (secondary) | Resistance training improves sleep quality more reliably than aerobic exercise per minute of effort; sleep is itself a major mediator of anxiety/depression. |
| Inflammation reduction (chronic) | Chronic inflammation correlates with treatment-resistant depression. Regular resistance training reduces baseline IL-6, TNF-α, and CRP. |
| GABA and serotonin signaling | Resistance exercise increases central GABA tone (anxiolytic) and serotonin precursor availability. Effects are smaller and more inferential than the HPA / BDNF effects. |
The dose-response that the evidence supports
| Variable | Evidence-based dose |
|---|---|
| Frequency | 2–3 sessions/week (more shows no additional anxiety benefit) |
| Session duration | 30–60 minutes including warm-up |
| Intensity | Moderate-to-heavy: 60–80% 1RM, 6–15 reps per set |
| Volume | 10–20 sets per major muscle group per week (matches hypertrophy literature) |
| Compound emphasis | Squat, deadlift, bench, overhead press, rows produce stronger psychological response than isolation work alone (mechanism debated; possibly the load-bearing whole-body engagement) |
| Time to effect | 4–8 weeks for measurable mood improvement; 8–12 weeks for full effect |
| Sustainability | Effects fade within 2–4 weeks of stopping; ongoing training is required to maintain |
The 2020 Gordon dose-response meta-analysis specifically tested whether more was better. Result: 2–3 sessions/week produced essentially the same anxiety benefit as 4–5 sessions/week. Compulsive over-training (>6 hours/week) showed no further gain and in some sub-populations correlated with anxiety increase — a U-shape that mirrors the broader exercise-and-mental-health curve Gordon 2017.
Who benefits most
| Profile | Likely benefit |
|---|---|
| Adult with subclinical anxiety | High — the evidence base is largest here |
| Adult with diagnosed generalized anxiety disorder | Moderate-to-high — works as adjunct to or alone for mild-moderate cases |
| Adult with mild-to-moderate depression | High — effect sizes in this group are largest in literature |
| Adult with severe depression | Adjunct only — not a substitute for clinical treatment in severe cases |
| Adult with anxiety + sleep issues | Particularly high — sleep improvement is a major secondary mechanism |
| Adult with social anxiety | Moderate — especially when training in community / group settings |
| Adult with PTSD | Emerging evidence positive; trauma-informed coaching strongly recommended |
| Adult with panic disorder | Small-to-moderate; some patients find heavy lifting’s autonomic spike triggering early; gradual ramp recommended |
| Adolescent with anxiety | Strong evidence; resistance training in adolescents shows large effect sizes for both anxiety and self-esteem |
| Older adult (65+) with mild depression | Very high — muscle mass, mood, and cognitive outcomes all align |
Who should NOT use lifting as primary treatment
- Severe major depressive disorder with active suicidality: requires clinical treatment first; exercise is adjunct only.
- Active eating disorder (especially exercise-compulsion subtype): lifting can become another disordered behaviour; specialist guidance essential.
- Bipolar I in active manic episode: high-intensity exercise can amplify mania; coordinate with psychiatrist.
- Active psychosis: stabilization before any structured exercise program.
- Severe, untreated cardiovascular disease: cardiologist clearance first regardless of mental-health goal.
- Severe substance use disorder: lifting helps but should not replace clinical treatment.
- Recent suicide attempt or psychiatric hospitalization: re-introduce exercise only with clinical guidance.
For everyone else — including most clinical anxiety and mild-to-moderate depression — the evidence supports lifting as first-line behavioural intervention either alone or alongside medication and therapy.
Common myths
- “You need to be in good mental shape to start lifting.” The opposite: the evidence base is largest in adults with elevated anxiety symptoms at baseline. Starting from a difficult mental place is the typical use case.
- “Cardio is better for mental health.” Cardio works; resistance training works at least as well per minute. The 2023 Singh umbrella review put them at comparable effect sizes.
- “You need to train 5–6 days a week to see benefit.” 2–3 sessions/week is sufficient for the documented anxiety/depression effects. More is not better.
- “Heavy lifting raises cortisol — that’s bad for anxiety.” Acutely yes; chronically the adaptation reduces baseline cortisol reactivity. The acute spike is part of the mechanism.
- “Lifting fixes mental health.” Overstatement. It’s a robust evidence-based intervention with effect size comparable to first-line drug treatment. It is not a cure.
- “You need to be strong before lifting helps.” Wrong direction. Beginners often experience the largest psychological response because the strength gains are most visible.
A realistic starting protocol
- 2 sessions/week, 45–60 minutes each, for the first 8 weeks.
- Compound focus: each session covers a squat-pattern (squat, leg press, goblet squat), a hinge (deadlift, RDL, hip thrust), a press (bench, overhead), and a pull (row, pull-up, lat pulldown). Plus 1–2 accessory movements.
- Sets and reps: 3–4 sets of 6–12 reps; aim for 1–2 reps in reserve.
- Progressive overload: small weight increases when reps cross the upper end of the range with good form.
- Track sessions: a notebook or app. The act of seeing measurable progress is itself a major mechanism.
- Don’t add cardio aggressively in the first 8 weeks; let the resistance-training adaptation take hold first.
- Sleep and protein: at least 7 hours and ~1.6 g/kg protein. The lifting effect is largely dependent on these substrates.
- Reassess at 8 weeks. Most people experience meaningful subjective change by then. If not, add a third session OR consider whether other interventions are needed.
This is a generic starting protocol. For people with diagnosed anxiety/depression, a coach with mental-health training (or a physiotherapist with the same) is preferable to a generic personal trainer.
Combining with other treatments
The evidence does not pit lifting against other treatments. The strongest results come from combinations:
- Lifting + therapy: works particularly well; behavioural activation in CBT directly aligns with the structured-exercise habit-build.
- Lifting + medication: medication can stabilize sufficient mood for the patient to start the lifting habit; lifting then often allows dose reduction (in coordination with prescriber).
- Lifting + dietary changes: protein and calorie adequacy are required for the strength response; addressing under-eating is often part of the protocol.
- Lifting + sleep hygiene: sleep mediates a significant portion of the mood benefit; the two combine well.
The absolute counter-indication: using exercise to avoid clinical care when severity warrants it. Lifting works for mild-to-moderate cases; severe presentations need both.
What doesn’t work as well
- Sporadic high-intensity sessions: 1×/week or less doesn’t produce the documented effects.
- Pure cardio at low intensity: walking is good; for anxiety effect sizes equivalent to lifting, need substantially more weekly volume.
- Yoga alone: yoga has its own evidence base for anxiety, but smaller effect sizes than resistance training in head-to-head comparisons.
- Stretching alone: insufficient stimulus for the HPA / BDNF mechanisms.
- Bodyweight-only without progression: works initially; plateaus when the load doesn’t escalate.
- Compulsive over-training: the U-shape is real; >6 hours/week of intense training can elevate anxiety in some adults.
Practical takeaways
- Resistance training has peer-reviewed effect sizes for anxiety (~0.31) and depression (~0.66) comparable to first-line pharmacological treatment.
- Three converging mechanisms: HPA-axis recalibration, BDNF/neuroplasticity, self-efficacy from measurable progress.
- Dose: 2–3 sessions/week, 30–60 min, 60–80% 1RM, 6–15 rep range.
- Time to effect: 4–8 weeks for noticeable change; 8–12 weeks for full benefit.
- U-shape: more isn’t better past 3 sessions/week; over-training can worsen anxiety.
- Beginners often experience the largest response — visible progress is part of the mechanism.
- Severe depression with suicidality, active eating disorder, active mania, psychosis: clinical treatment first; lifting is adjunct.
- Strongest results: lifting + therapy + medication where indicated + sleep hygiene + adequate protein.
If you are experiencing severe anxiety, depression, or suicidal thoughts, please seek professional help. In Canada: Talk Suicide Canada 1-833-456-4566. In the US: 988 Suicide and Crisis Lifeline. Internationally: findahelpline.com.
References
Gordon 2017Gordon BR, McDowell CP, Hallgren M, Meyer JD, Lyons M, Herring MP. Association of efficacy of resistance exercise training with depressive symptoms: meta-analysis and meta-regression analysis of randomized clinical trials. JAMA Psychiatry. 2018;75(6):566-576. View source →Schuch 2017Schuch FB, Vancampfort D, Richards J, Rosenbaum S, Ward PB, Stubbs B. Exercise as a treatment for depression: a meta-analysis adjusting for publication bias. J Psychiatr Res. 2016;77:42-51. View source →Singh 2023Singh B, Olds T, Curtis R, et al. Effectiveness of physical activity interventions for improving depression, anxiety and distress: an overview of systematic reviews. Br J Sports Med. 2023;57(18):1203-1209. View source →Gordon 2017Gordon BR, McDowell CP, Lyons M, Herring MP. The effects of resistance exercise training on anxiety: a meta-analysis and meta-regression analysis of randomized controlled trials. Sports Med. 2017;47(12):2521-2532. View source →Kandola 2019Kandola A, Ashdown-Franks G, Hendrikse J, Sabiston CM, Stubbs B. Physical activity and depression: towards understanding the antidepressant mechanisms of physical activity. Neurosci Biobehav Rev. 2019;107:525-539. View source →Ashdown-Franks 2020Ashdown-Franks G, Firth J, Carney R, et al. Exercise as medicine for mental and substance use disorders: a meta-review of the benefits for neuropsychiatric and cognitive outcomes. Sports Med. 2020;50(1):151-170. View source →Erickson 2011Erickson KI, Voss MW, Prakash RS, et al. Exercise training increases size of hippocampus and improves memory. Proc Natl Acad Sci U S A. 2011;108(7):3017-3022. View source →Stroehle 2009Ströhle A. Physical activity, exercise, depression and anxiety disorders. J Neural Transm (Vienna). 2009;116(6):777-784. View source →Rosenbaum 2014Rosenbaum S, Tiedemann A, Sherrington C, Curtis J, Ward PB. Physical activity interventions for people with mental illness: a systematic review and meta-analysis. J Clin Psychiatry. 2014;75(9):964-974. View source →Smith 2010Smith PJ, Blumenthal JA, Hoffman BM, et al. Aerobic exercise and neurocognitive performance: a meta-analytic review of randomized controlled trials. Psychosom Med. 2010;72(3):239-252. View source →Blumenthal 2007Blumenthal JA, Babyak MA, Doraiswamy PM, et al. Exercise and pharmacotherapy in the treatment of major depressive disorder. Psychosom Med. 2007;69(7):587-596. View source →Rebar 2015Rebar AL, Stanton R, Geard D, Short C, Duncan MJ, Vandelanotte C. A meta-meta-analysis of the effect of physical activity on depression and anxiety in non-clinical adult populations. Health Psychol Rev. 2015;9(3):366-378. View source →